Chemoembolization, Ablation, And Other Liver Cancer Treatments
As vascular experts, interventional radiologists are uniquely skilled in using the vascular system to deliver targeted treatments via catheter throughout the body. In treating cancer patients, interventional radiologists can attack the cancer tumor from inside the body without medicating or affecting other parts of the body.
Tumors need a blood supply, which they actively generate, to feed themselves and grow. Interventional radiologists can attack the cancer tumor from inside the body without medicating or affecting other parts of the body by using embolization and heat-based therapies.
Embolization is a well-established interventional radiology technique that is used to treat trauma victims with massive bleeding, to control hemorrhage after childbirth, to decrease blood loss prior to surgery and to treat tumors. In treating cancer patients, interventional radiologists use embolization to cut off the blood supply to the tumor (embolization or chemoembolization), deliver radiation to a tumor (radioembolization), or combine this technique with chemotherapy to deliver the cancer drug directly to the tumor (chemoembolization).
Additionally, interventional radiologists can use imaging to guide them directly to the tumor through the skin to administer radiofrequency heat to "cook" and kill the cancer cells (radiofrequency ablation), microwave ablation, or cyroablation to freeze the tumor.

Chemoembolization
Chemoembolization is a minimally invasive treatment for liver cancer that can be used when there is too much tumor to treat surgically or through heat-based methods such as RFA, Microwave or cryoablation. Sometimes, this may be used in combination with RFA, microwave ablation or other treatments.
Chemoembolization delivers a high dose of cancer-killing drug (chemotherapy) directly to the organ while depriving the tumor of its blood supply by blocking, or embolizing, the arteries feeding the tumor. The interventional radiologist threads a catheter up the femoral artery in the groin into the blood vessels supplying the liver tumor. By blocking the blood flow to the tumor, a higher dose of chemotherapy drug can be used. This allows less of the drug to circulate to the healthy cells in the body. An overnight hospital stay is required, and most patients can go home the following morning. Patients typically have lower than normal energy levels for about week or two afterwards.
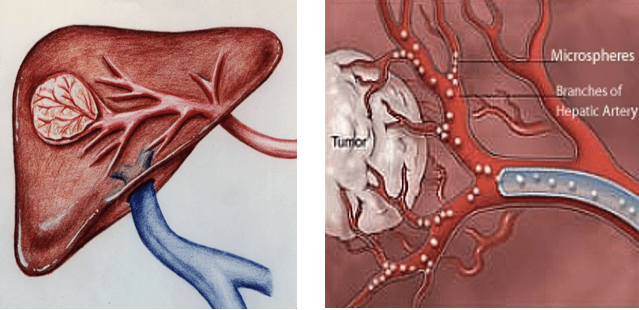
Chemoembolization is a palliative, not a curative, treatment. It can be extremely effective in treating primary liver cancers, especially when combined with other therapies. Chemoembolization has also shown promising results with some types of metastatic tumors.
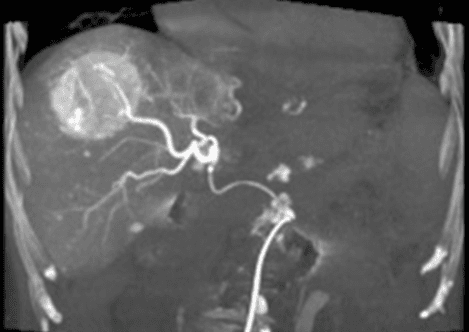
In the image above, a catheter is positioned in the hepatic artery and x-ray dye injected showing the large liver tumor at the top right of the image. The Interventional Radiologist will block the blood supply and deliver high dose chemotherapy at the same time to kill the tumor.
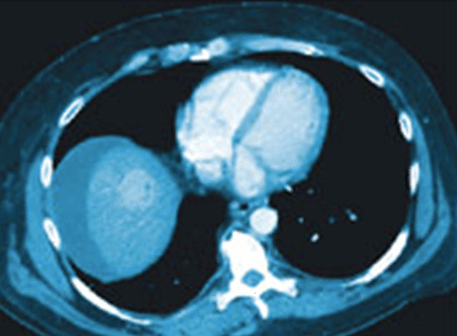
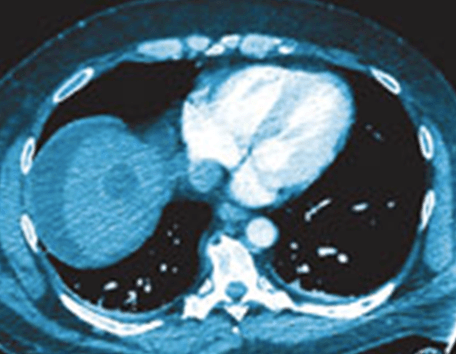
BEFORE – Bright spot on right side of image is the viable “alive” liver tumor
AFTER – Bright spot is now a dark hole indicating necrosis or “dead” tumor
Radiofrequency and Microwave Ablation
For inoperable liver tumors, radiofrequency ablation (RFA) or microwave ablation offers a nonsurgical targeted treatment that kills the tumor cells with heat, while sparing the majority of healthy liver tissue. This treatment is usually easier on the patient than systemic therapy.
In this procedure, the interventional radiologist guides a small needle through the skin into the tumor. From the tip of the needle, energy is transmitted to the tip of the needle, where it heats the tissues. This eventually kills the tumor tissue. This treatment is FDA approved for killing certain solid organ tumors and can be curative.
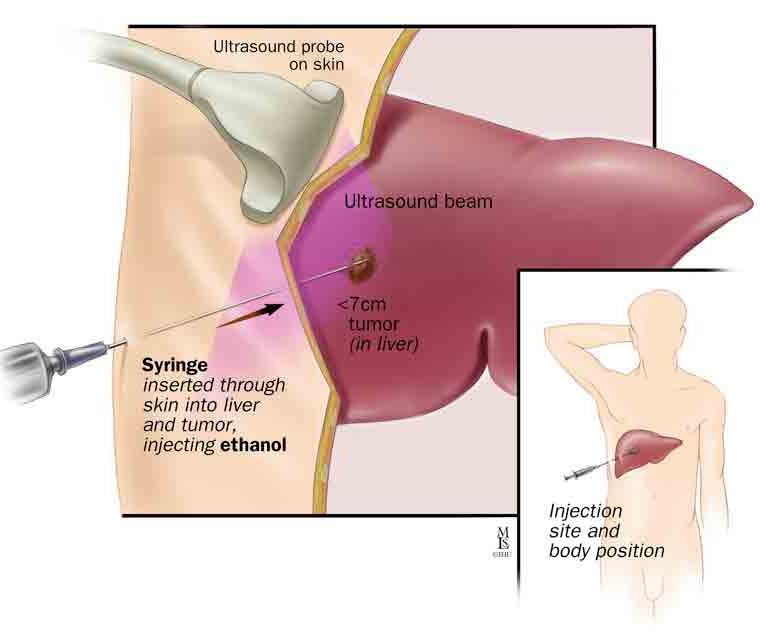
Cryoablation
Cryoablation is a method of “freezing” a tumor. It is similar to RFA or microwave ablation in that the energy is delivered directly into the tumor by a probe that is inserted through the skin. But rather than killing the tumor with heat, cryoablation uses an extremely cold gas to freeze it. This technique has been used for many years by surgeons in the operating room, but in the last few years, the needles have become small enough to be used by interventional radiologists through a small nick in the skin, without the need for an operation. The "ice ball" that is created around the needle grows in size and destroys the frozen tumor cells. This technique is most often used to kill inoperable kidney or renal tumors.
Any patient with a renal tumor that may not be a candidate for surgery (nephrectomy or partial nephrectomy) may be considered for ablative therapy by either cryoablation or microwave ablation.
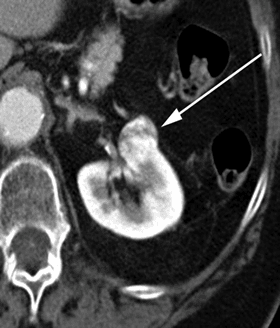
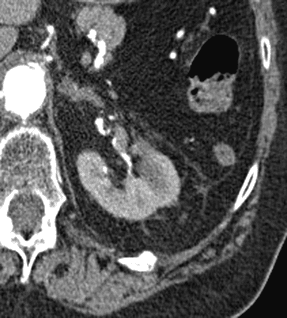
BEFORE AFTER
-
“I especially owe a debt o f gratitude to Dr. Petruzzi and Dr. Adler for their skills and encouragement. ”
- Anonymous -
“I’m so grateful to have Dr. Petruzzi and his staff as part of the medical team treating and dealing with my newly diagnosis of PAD. He’s very sensitive, respectful, and most of all compassionate. Thanks for all you do ALWAYS! ”
- Anonymous -
“Dr. Jacinto Camarena is very knowledgeable, and he takes the time to fully answer all your questions and takes the time to explain everything. I highly recommend him. Also, the staff at AMI is great. ”
- Anonymous -
“It was a COVID-safe environment and the staff was very welcoming and professional. Dr. Watts has a vast knowledge of vascular issues and discusses the value of empirical evidence to support a sound strategy of treatment. His personality is positive, and his analysis is patient-specific. Highly recommend ”
- Anonymous -
“Dr. Schmidling was very patient and caring. He explained the process every step of the way and I never felt rushed or ignored. Great doctor and support staff! ”
- Anonymous -
“I saw Dr. Kim at the Brick Office. He was extremely knowledgeable, compassionate, and attentive to my medical issues. He was very patient explaining things to me using pictures and diagrams. Dr. Kim treated me like I was the most important patient he has! I am so happy to be his patient and I feel that I am in competent hands! Thank you, AMI for having ... ”
- Anonymous

